Fallstudie 008: Die pragmatisch stabile Praxis
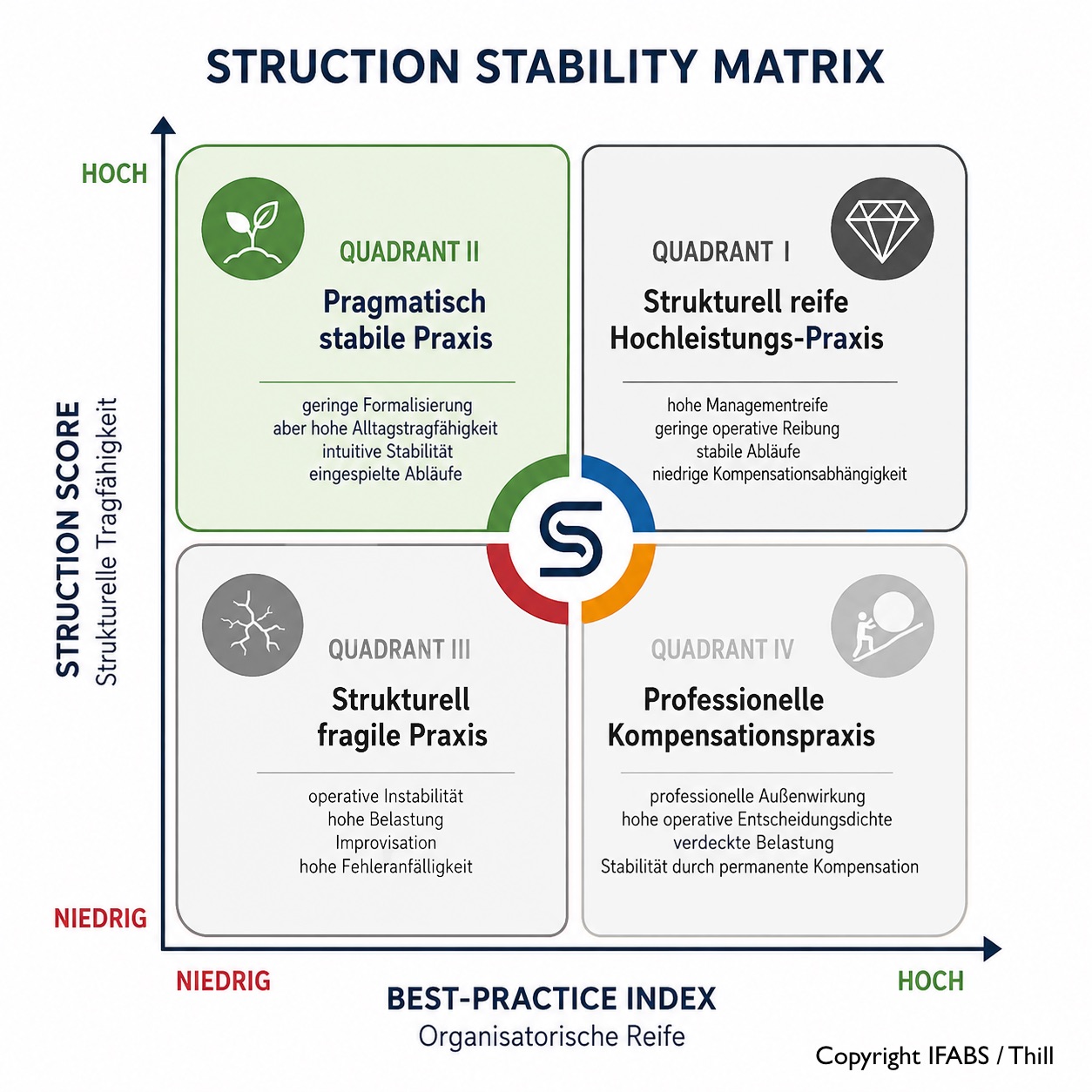
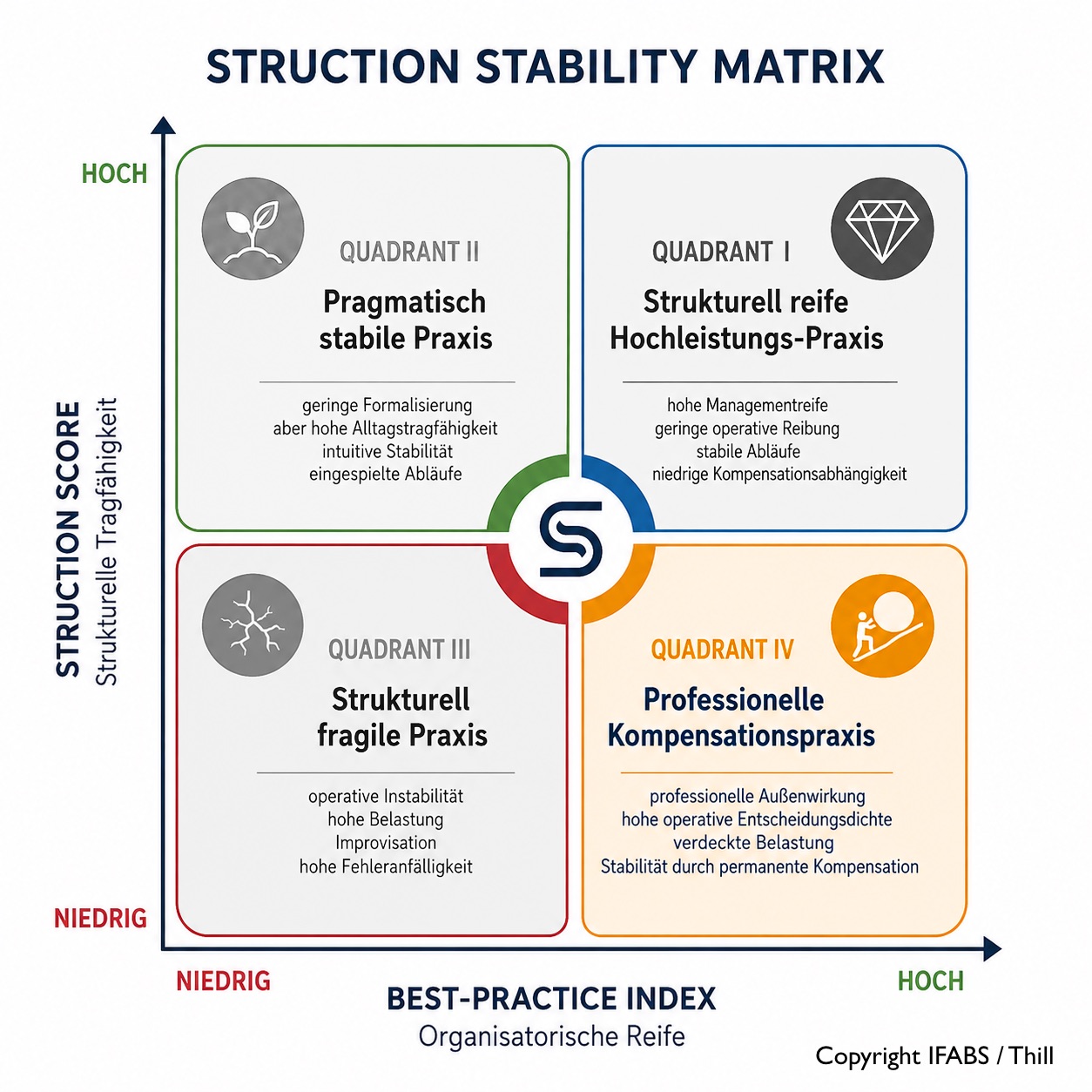
Diese Fallstudie basiert auf dem Struction-Ansatz, der ausführlich im Buch „Die unsichtbare Belastung der Arztpraxis: Warum Organisation allein nicht genügt – Ein neuer Blick auf Praxisstabilität, Entscheidungsdichte und strukturelle Tragfähigkeit“ beschrieben wird. Dort werden die theoretischen Grundlagen, die Struction Stability Matrix, die Bewertungslogik des Struction Score sowie die Zusammenhänge zwischen organisatorischer Reife und struktureller Tragfähigkeit detailliert dargestellt.
Continue reading “Die Praxis, die Belastung absorbierte statt eskalierte · Struction Diagnostics: Strukturelle Fallstudien aus Haus- und Facharztpraxen”